
Our 2026 Doctor Engagement Barometer asked 500 Australian doctors - evenly split between GPs and Specialists - how their experience with pharma has changed over the past three to five years.
While specialists are more likely than GPs to report clear improvements, differences also emerge by generation, with younger doctors tending to be more positive than experienced physicians.
In this article we explore:
Pharma teams may feel their omnichannel investments are paying off, but doctors’ experiences suggest a more mixed picture.
Since 2020, pharma teams have invested heavily in sophisticated engagement strategies, diversified touchpoints, and digital transformations. From an internal viewpoint, these actions look like momentum.
Yet when doctors answer a simple question in our 2026 survey - has my experience with pharma over the last three to five improved? – many say no. While activity has increased, perceived value has lagged, and that gap matters commercially.
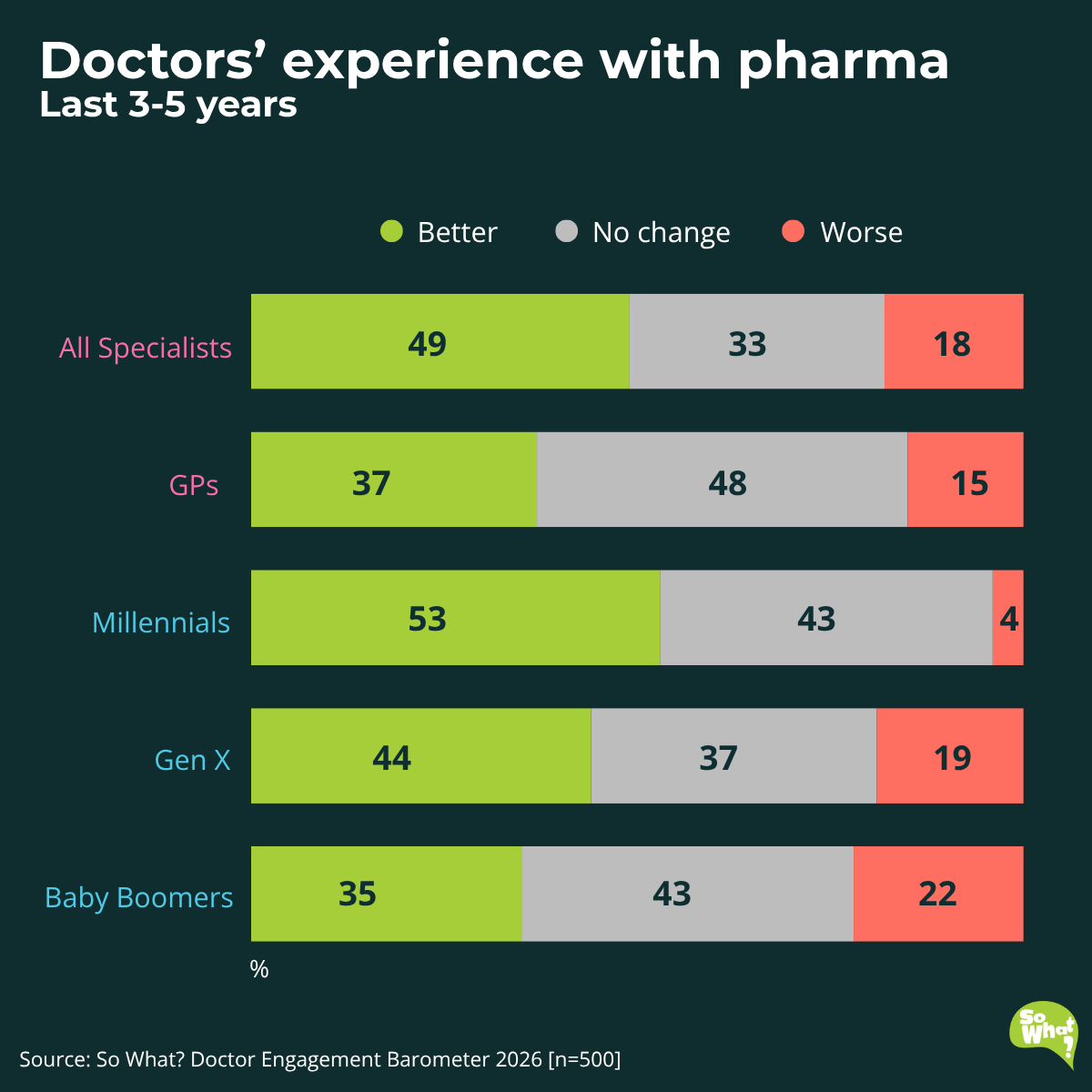
The data shows that doctor experience is improving unevenly. Specialists demonstrate a more positive engagement experience, with 49% confirming an enhancement in their interactions with pharma. However, 33% report no change, and 18% indicate a decline.
Among GPs, the picture is weaker: only 37% of GPs report an improvement, with a considerable 48% experiencing no change. Furthermore, 15% report a decline in engagement quality. For teams whose current market volume depends on GPs, this is not a neutral finding.
When we look at the data by generation, Millennials have the highest positive sentiment, with 53% highlighting improvements. Gen X follows with 44%, though 19% feel engagement has worsened. Baby Boomers are the least positive, with only 35% reporting better interactions, and 22% experiencing a decline. These insights highlight the importance of tailoring strategies across different age groups to ensure relevance.
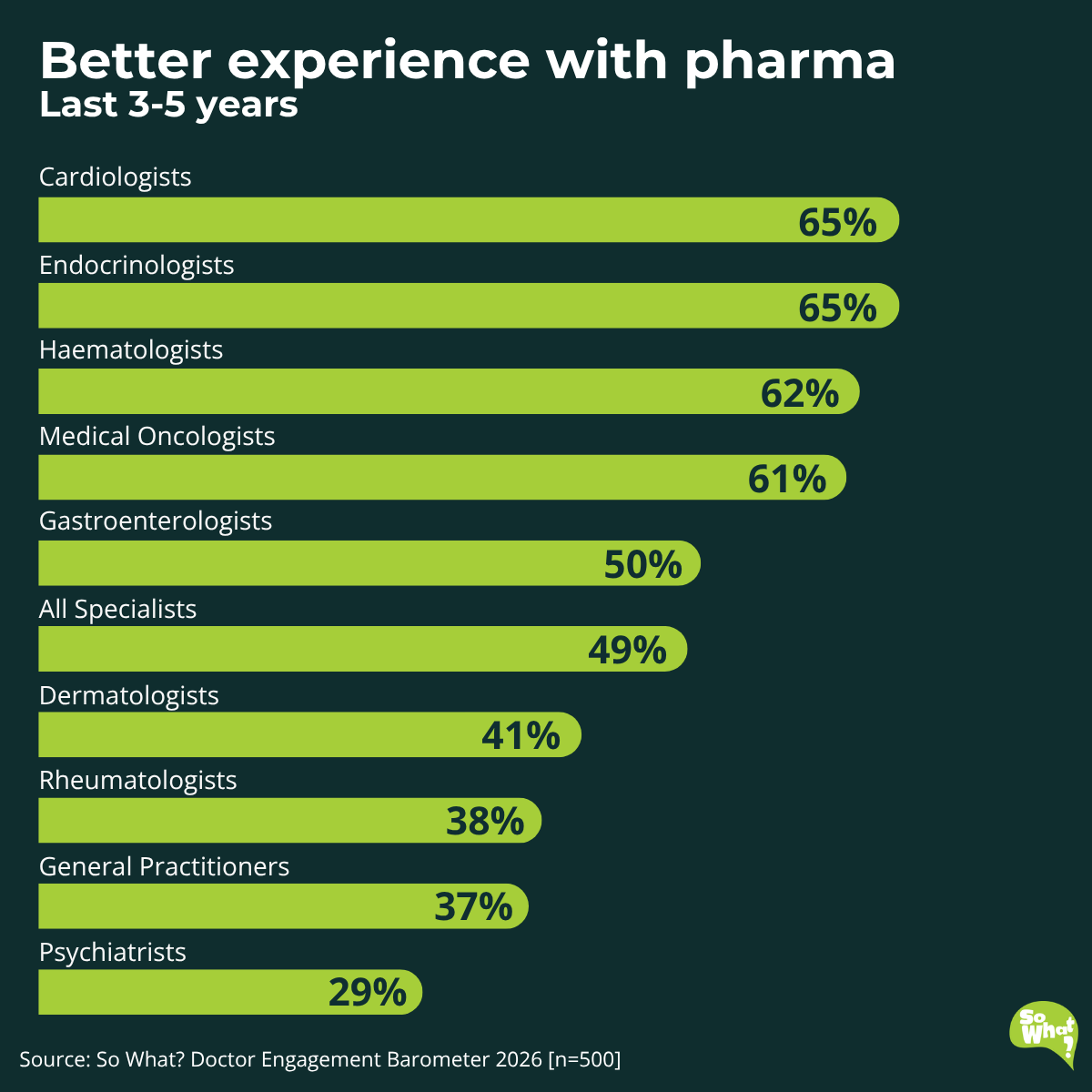
Cardiologists and endocrinologists lead, with 65% reporting a better experience. Haematologists (62%) and medical oncologists (61%) follow closely. At the other end, psychiatrists (29%), GPs (37%), and rheumatologists (38%) lag well behind.
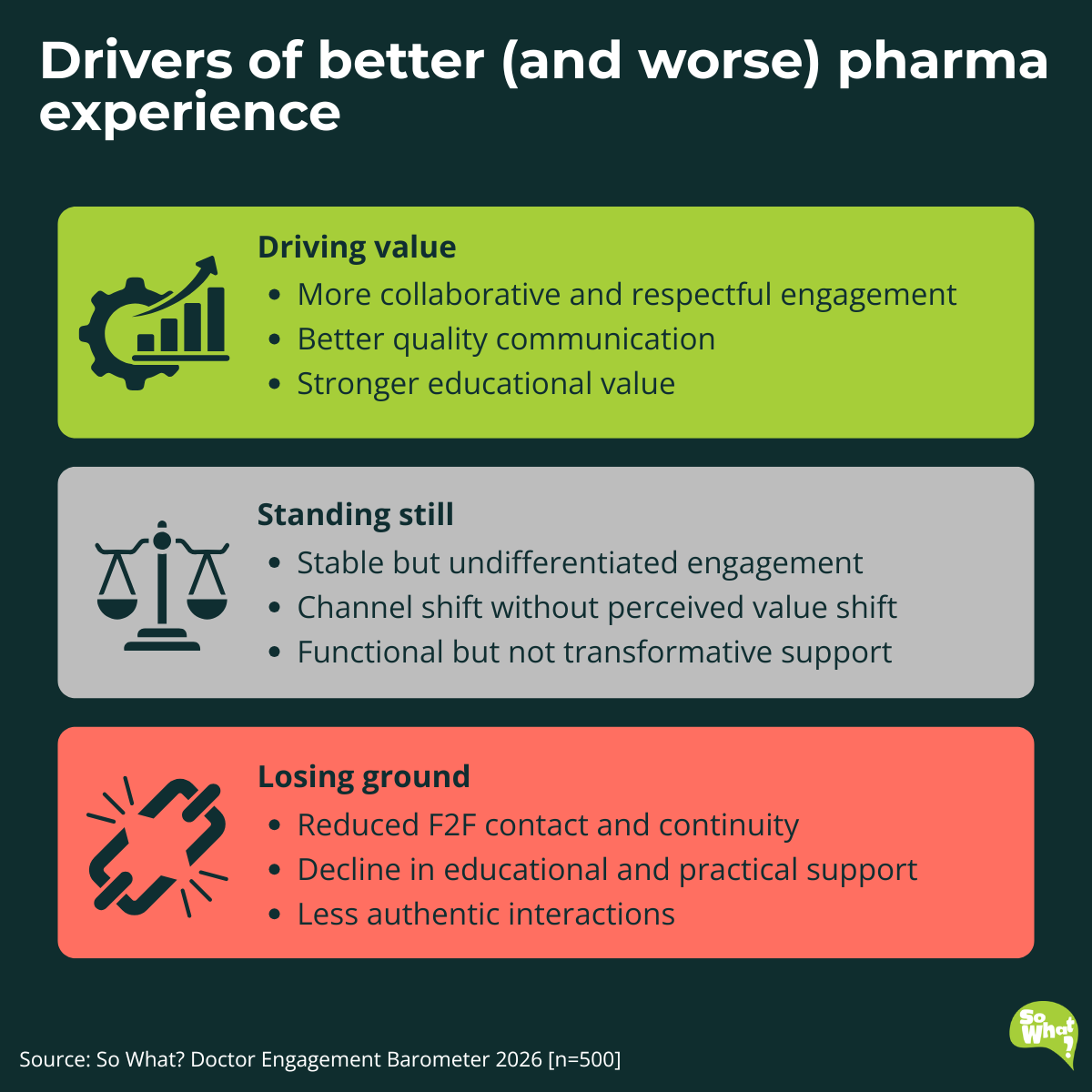
When we look at what separates the "better" group from those reporting “no change”, the difference is not frequency of contact. It is the strength and relevance of what is delivered. Doctors in the "better" group say pharma provides clear and useful information, practical guidance they can apply in real cases, and genuine support with access and reimbursement.
Doctors rarely credit improvement to seeing more sales representatives or receiving more emails. Many actively value less frequent but more purposeful interaction.
Nearly half of all GPs (48%) sit in the "no change" group despite five years of digital transformation and omnichannel investment. They see the reps and receive the emails but describe the net impact as background noise.
Those reporting "worsened" experiences point to less face-to-face contact, fewer sponsored educational events and engagement that feels more transactional than before.
The data highlights a mixed reality. Specialists and younger doctors are feeling more engaged, but GPs and more experienced doctors aren’t seeing the same benefit. Engagement may be increasing, but for many core prescribers, it’s not translating into something genuinely useful in their day-to-day practice.
Three key takeaways to reflect on:
1. Activity can create an illusion of progress. Increased engagement does not always mean increased value. The quality and relevance of interactions are essential. If doctors experience activity as only modestly helpful, the net impact on experience may be neutral or worse.
2. The biggest commercial risk sits in the "no change" middle. 48% of GPs report no change after years of omnichannel investment. A high-frequency, low-depth perception is a strategic liability. Shifting this group requires moving toward greater utility, not more noise.
3. Where data and access converge, practical support sets you apart. In crowded therapy areas, clinical evidence and PBS status often look similar across competitors. Here, the perception that a company genuinely makes practice easier becomes a critical differentiator. A plateaued experience is a missed competitive advantage.
Looking ahead, the focus should be on delivering practical, useful engagement and support that genuinely helps doctors in their day-to-day decisions. There are four actionable steps pharma teams can take to better support doctors.

1. Prioritise activities by impact: Conduct a thorough review of your current engagement plan. Identify which initiatives truly add value and solve real clinical problems, and which don’t. Aim to align your activities with the distinct needs of both specialists and GPs.
2. Identify areas for improvement: Analyse feedback and data to pinpoint where engagement strategies are falling short. Tailor your approach to deliver more tangible benefits, and in doing so, bridge any customer experience gaps.
3. Shift from informing to supporting. Move beyond simply delivering information. Develop tools and resources that can be seamlessly integrated into daily practice, providing practical, actionable support that doctors find genuinely useful. This shift can help convert passive engagement into active collaboration.
4. Treat engagement as a strategic priority: View improving doctor interactions as an opportunity for growth. By addressing the disparities in experiences, you can not only maintain but enhance relationships, positioning your brand as a responsive and thoughtful partner in healthcare delivery.
Our data provides a market-level view of where Australian doctors sit overall. What it does not tell you is how your brand, therapy area or engagement model maps onto this picture. Your customers’ experiences are shaped by the support they receive, the channels you use, and the clinical problems you do or don't help them solve.
Three questions worth taking into your next planning discussion:
1. Among the prescribers most important to your brand, how many would currently say their experience with your company is "better"? How many would say "no change" or worse?
2. Which of your current activities, if switched off tomorrow, would those prescribers genuinely miss?
3. Where is your engagement delivering felt, practical value, and where is it landing as background noise?
The gap between activity and impact is where the real commercial opportunity lives.
Our May article unpacks ‘The Coordination Gap’: how inconsistencies across rep, MSL and digital touchpoints reduce the impact of pharma engagement - and how to fix it.
These insights come from The So What? Doctor Engagement Barometer 2026 - an independent national online study of n=500 doctors (n=250 GPs and n=250 specialists across 20+ specialties). The research explores doctors’ experience with pharmaceutical companies. Data was from December 2025 to February 2026.